Abstract
Although the BCL2 inhibitor venetoclax have been transformative in the management of AML, therapeutic resistance and relapse are frequently observed. In light of the urgent need to uncover novel therapeutic options in AML, we sought to study the potential role of ironomycin (AM5), a recently described small molecule that induces cell death through the sequestration of lysosomal iron.
To evaluate the effects of ironomycin in AML, we chose a diverse panel of AML cell lines. These data showed a potent and dose-dependent effect, on proliferation, cell cycle progression and survival at a nanomolar range. In contrast to venetoclax, the cell death induced by ironomycin did not result in potent caspase activation or PARP1 cleavage. Neither the caspase inhibitor Z-VAD-fmk nor the necroptosis inhibitor necrostatin-1 did prevent cell death. Consistent with previous observations, we found that ironomycin accumulates in the lysosomes of AML cells leading to a sequestration of iron in this organelle but inhibitors of canonical ferroptosis, including ferrostatin-1 and liproxstatin-1 failed to prevent the activity of ironomycin.
To gain greater insight into the molecular mechanism of ironomycin in AML cells, we performed a genome-wide positive-selection resistance screen under ironomycin selection pressure and collected several samples for sequencing. We found nine genes whose knock out conferred resistance to the drug. Interestingly, these data implicated key components of mitochondrial metabolic pathways, including phosphoglycolate phosphatase (PGP), a central phosphatase involved in glycolysis and pentose phosphate pathway (PPP) regulation and Hexokinase 2 (HK2), the first enzyme of glycolysis.
Mass-spectrometry metabolomics analyses highlighted that ironomycin treatment significantly reduced key components of the TCA cycle and consequently the reducing agent nicotinamide adenine dinucleotide (NADH) and increased the intracellular concentration of amino acids. These data were corroborated with RNAseq showing a mitochondrial stress response mediated through the Activating Transcription Factor 4 (ATF4) and its paralog Activating Transcription Factor 5 (ATF5). As mitochondria are major hubs of iron utilization for oxidative respiration, we used Mass-spectrometry to measure mitochondrial iron load. We observed a rapid and dose-dependent decrease in mitochondrial iron after treatment mirroring the iron sequestration into the lysosomes and inducing the mitochondrial dysfunction.
We next examined the ultrastructural appearance of mitochondria after ironomycin using transmission electron microscopy and observed a dramatic alteration of the structural integrity of mitochondria resulting in abnormal cristae, matrix density changes and mitochondrial membrane blebbing. In cells lacking BAX and BAK, the two main effectors of mitochondrial membrane permeabilization, structural changes and cell death were almost completely rescued but cell proliferation was still markedly affected, consistent with a BAX/BAK dependent cell death following mitochondrial iron deprivation. In vivo imaging confirmed that BAX activation occurred after 30 hours of treatment and preceded cell death, but we observed some major differences with canonical apoptosis induced by venetoclax. First, the structural alterations were clearly distinct. Next, delay between MOMP and cell death was significantly longer and caspase inhibitors weakly delayed cell death. Finally, BCL2 overexpression and P53 deletion did not rescue ironomycin cell death.
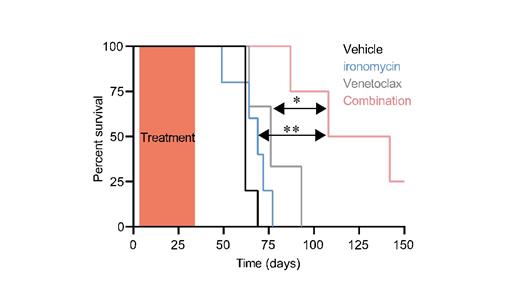
These non-canonical features prompted us to assess the efficacy of the combination between ironomycin and venetoclax. In vitro experiment on AML cell lines found a high synergy between the two drugs. In vivo experiments on xenotransplanted mice confirmed the efficacy of the combination, which was associated with a significant increase in mice survival in comparison with the controls (Figure). Finally, primary AML samples from patients clinically resistant or refractory to venetoclax were sensitive to ironomycin in monotherapy and even more in combination with venetoclax.
These results demonstrate that the novel mechanism of ironomycin action can be leveraged to resensitize AML cells to venetoclax and substitute for cytotoxic drugs as a more effective therapeutic combination in the salvage setting.
Huang: The Walter and Eliza Hall Institute of Medical Research: Patents & Royalties: Employee of the Walter and Eliza Hall Institute and eligilble for payments in relation to venetoclax. Wei: Novartis, Celgene, AbbVie, Servier, AstraZeneca, and Amgen: Research Funding; Novartis, Janssen, Amgen, Roche, Pfizer, Abbvie, Servier, BMS, Macrogenics, Agios, Gilead: Membership on an entity's Board of Directors or advisory committees; Astellas: Honoraria.

This feature is available to Subscribers Only
Sign In or Create an Account Close Modal